Is shoulder pain stopping you from playing your favorite sport or achieving your personal fitness goals? Chances are, if you are experiencing shoulder discomfort or pain, you’ll have to alter your lifestyle to accommodate this dysfunction. Shoulder pain can occur in a multitude of ways and is prevalent in 21% of the general population (1,2) with 40% of that population having injuries persisting for at least one year (3). The treatment measures of shoulder pain can accumulate to an estimated annual cost of $39 billion (4).
Shoulder injuries have many different mechanisms or pathologies ranging from acute trauma to chronic overuse injuries. Acute trauma typically comes from a direct force, such as falling directly on the shoulder, or from an indirect force, such as landing on an outstretched hand. Either of these mechanisms may result in fractures of the humerus, clavicle, scapulae and glenoid fossa, or dislocations and tears of the capsular ligaments or labrum. However, the most commonly seen injuries in athletes or the active population stem from overuse syndromes.
Overuse Injuries
Overuse injuries (aka cumulative trauma disorders) are any type of muscular or joint injury caused by repetitive stress that surpasses the body’s natural repair processes (i.e., tendonitis, stress fractures). Overuse injuries of the shoulder are common among athletes who consistently perform overhead movement patterns (i.e., baseball pitchers, swimmers, tennis players) and individuals who repeatedly work with their arms raised (i.e., painters, construction workers) (5-9). Among the overuse injuries, shoulder impingement is the most prevalent diagnosis accounting for 40-65% of reported shoulder pain (10).
Common symptoms of shoulder overuse injuries include (11):
- Minor pain during activity and at rest
- Pain observed at the top or front of the shoulder during overhead activity (i.e., overhead presses) or during chest activities (i.e., incline bench press)
- Tenderness on the lateral aspect (outside) of the shoulder
- Loss of strength and range of motion (ROM)
- Pain during throwing motions
Poor Posture
In addition to overuse injuries, individuals who exhibit poor static posture of the upper body are at risk for shoulder dysfunction. A common postural distortion of the upper body identified by Janda is the Upper Crossed Syndrome (UCS) and is characterized by protracted shoulders and a forward head (12). UCS generally involves tightness (overactivity) within the anterior chest region (pectoralis major/minor), latissumus dorsi, and cervical extensors (sternocleidomastoid, levator scapulae, scalenes), coupled with lengthening and weakening (underactivity) of the mid-and-upper back muscles (mid/lower trapezius, serratus anterior, rotator cuff) and deep cervical flexors. Individuals who sit for extended periods working on a computer may be at risk for developing upper body dysfunction and poor posture if certain precautions are not made such as taking frequent breaks and working at an ergonomically sound work station (13).
Exercise Selection
Similar to overuse and poor static posture, improper exercise selection can also contribute to shoulder dysfunction. For example, if a baseball pitcher tries to increase velocity of his pitches by only strengthening the superficial muscles of the shoulder (prime movers) that produce internal rotation (pectoralis major, latissimus dorsi) more than the stabilizers/external rotators of the shoulder (infraspinatus, supraspinatus, teres minor), these stabilizers become reciprocally inhibited (underactive) and fail to stabilize the glenohumeral joint during the throwing motion. Without adequate stability the athlete may develop a subacromial impingement, leading to subacromial bursitis, rotator cuff tendonitis, and possible tears of the external rotators (14).
Another example of poor exercise selection involves the over reliance on uniplanar, isolated resistance training exercises. Athletes and fitness enthusiasts oftentimes place too much emphasis on uniplanar exercises strictly focusing of concentric force production (e.g., presses and pulls) while neglecting total-body movements that integrate the entire kinetic chain (lower body, core, upper body) in multiple planes of motion (sagittal, frontal, transverse). Everyday activity occurs in all three planes of motion (front-to-back, side-to-side, and rotational) and only training in one plane (predominately the sagittal plane) will not effectively improve the individual’s ability to move in a coordinated fashion in the frontal and transverse planes. This form of program design may lead to muscle imbalance and faulty movement patterns increasing the individual’s risk of injury and/or joint dysfunction.
Using these two examples, fitness professionals should design exercise programs from an integrated (all-inclusive) perspective. An integrated exercise program encompasses both uniplanar and multiplanar movements; single, compound and total-body exercises; and adequately targets on all muscle groups (prime movers and stabilizers).
Shoulder Injury Prevention Strategies
If a client presents pain or dysfunction the fitness professional should never attempt to diagnose the problem but rather refer his or her client to a qualified medical professional. However, utilizing various movement screens, fitness professionals should assess their clients to identify potential muscles imbalances (muscle weakness and muscle tightness) and faulty movement patterns and subsequently implement a corrective exercise strategy to proactively address these concerns. For a list of comprehensive movement screens and corrective strategies for the shoulder complex see NASM’s Corrective Exercise Specialist.
Following a comprehensive fitness assessment (including a battery of movement screens), fitness professionals should implement a corrective exercise program that is individualized for their client:
- Step 1: Inhibitory techniques (self-myofascial release) should be used to decrease tension and effects of latent trigger points of the overactive muscles surrounding the shoulder complex.
- Step 2: Static stretching should be performed for a minimum of 30 seconds on identified overactive muscles to help facilitate optimal joint ROM and muscle extensibility.
- Step 3: Isolated strengthening exercises should be used to facilitate the underactive muscles of the scapulae. Auditory and tactile feedback while performing these exercises can also help develop neuromuscular activation with proper kinetic chain positioning and control.
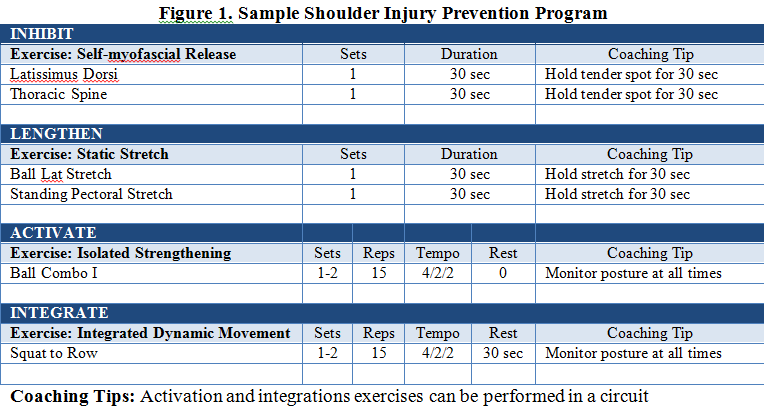
- Step 4: Lastly, exercises are progressed by incorporating activities that integrate the entire kinetic chain (multijoint, compound movements). During these exercises clients should be instructed to maintain scapular retraction, depression, and posterior tilting while limiting winging by keeping the scapula on the costal surface. Refer to Figure 1 for an example shoulder corrective exercise program.
References:
1. Bongers PM. The cost of shoulder pain at work. BMJ. 2001;322(7278):64-65.
2. Urwin M, Symmons D, Allison T, Busby H, Roxby M, Simmons A, Williams G. Estimating the burden of musculoskeletal disorders in the community: the comparative prevalence of symptoms at different anatomical sites, and the relation to social deprivation. Ann Rheum Dis.1998;57(11):649-655.
3. Van der Heijden G. Shoulder Disorders: A state of the art review. Baillieres Best Pract Res Clin Rheumatol.1999;13(2):287-309.
4. Johnson M, Crosley K, O'Neil M, Al Zakwani I. Estimates of direct health care expenditures among individuals with shoulder dysfunction in the United States. J Orthop Sports Phys Ther. 2005;35(1):A4-PL8.
5. Wilk KE, Macrina LC, Cain EL, Dugas JR, Andrews JR. The recognition and treatment of superior labral (slap) lesions in the overhead athlete. Int J Sports Phys Ther. 2013 Oct;8(5):579-600.
6. Reinold MM, Curtis AS. Microinstability of the shoulder in the overhead athlete. Int J Sports Phys Ther. 2013 Oct;8(5):601-16.
7. Reinold MM, Gill TJ, Wilk KE, Andrews JR. Current concepts in the evaluation and treatment of the shoulder in overhead throwing athletes, part 2: injury prevention and treatment. Sports Health. 2010 Mar;2(2):101-15.
8. Reinold MM, Gill TJ. Current concepts in the evaluation and treatment of the shoulder in overhead-throwing athletes, part 1: physical characteristics and clinical examination. Sports Health. 2010 Jan;2(1):39-50.
9. Stenlund B, Lindbeck L, Karlsson D. Significance of house painters' work techniques on shoulder muscle strain during overhead work. Ergonomics. 2002 May 15;45(6):455-68.
10. van der Windt DA, Koes BW, Boeke AJ, Deville W, De Jong BA, Bouter LM. Shoulder disorders in general practice: prognostic indicators of outcome. Br J Gen Pract.1996;46(410):519-523.
11. American Academy of Orthopaedic Surgeons. http://orthoinfo.aaos.org/topic.cfm?topic=a00032. Accessed November 12, 2013.
12. Janda V. Muscles and Motor Control in Cervicogenic Disorders. In: Grant R, ed. Physical Therapy of the Cervical and Thoracic Spine. St. Louis, MO: Churchill Livingstone; 2002:182–99.
13. Cho CY, Hwang YS, Cherng RJ. Musculoskeletal symptoms and associated risk factors among office workers with high workload computer use. J Manipulative Physiol Ther. 2012 Sep;35(7):534-40.
14. Cowderoy GA, Lisle DA, O'Connell PT. Overuse and impingement syndromes of the shoulder in the athlete. Magn Reson Imaging Clin N Am. 2009 Nov;17(4):577-93.