Figure skaters are grace and skill on ice. These athletes’ determination, athleticism, and work ethic cannot be overstated, as the sport of competitive figure skating is both physically and mentally demanding. It is through undeniable grit, dedication, and hundreds, if not thousands, of hours on the ice that these athletes are able to complete incredibly amazing and beautiful feats such as triple and even quadruple jumps. And figure skaters continue to push the envelope striving to perfect even more difficult technical skills. Due to the competitive nature and rigorous training methods required, competitive figure skaters experience their fair share of both acute and chronic injuries; such as bruising and swelling from a fall (acute) or suffer from overuse (chronic) issues like tendinitis or stress fractures. However, research has shown chronic injuries are more prevalent than acute injuries during individual skating, and not surprisingly, the area most commonly injured is the lower extremity (1,2,3). It is important to note acute injuries are more common in pairs and synchronized skating (2). This difference is most likely attributed to the close proximity of the skaters during technical skills which can result in collisions and falls during a lift.
Foot and Ankle Injuries
The foot and ankle complex takes the brunt of the injuries (1,3). Injuries to the foot are due to the tremendous forces applied to the foot while jumping and the restrictive design of the figure skating boot (2,3). Some examples of foot-related injuries include bursitis to the medial malleolus, hammer toes, corns, bunions and warts, often caused by overly stiff figure skating boots and overuse (i.e., constant jumping) (2,3).
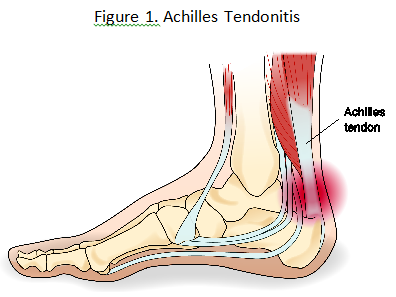
Achilles Tendonitis
Another common injury experienced by figure skaters is Achilles tendonitis (Figure 1). The gastrocnemius complex, which consists of the gastrocnemius and soleus (calf) muscles share the Achilles tendon to insert on the base of the calcaneus (heel bone). Signs and symptoms of Achilles tendonitis include pain during physical activities or at rest, inflammation, swelling, and thickening of the tendon. Mechanisms of injury include overuse, poorly fitted shoes, and eccentric loading (4). Jumping and running are common causes of Achilles tendonitis, and specifically figure skaters may develop Achilles tendonitis because of overtraining, repetitive jumping, and pressure exerted from the top of the boot (2,4).
Achilles tenosynovitis is another common injury to the Achilles tendon experienced by figure skaters (2,3). The covering of the Achilles tendon is called the tenosynovium, a fluid-like sheath allowing for the tendon to slide under the skin. Constant rubbing and pressure from the boot can irritate the tenosynovium leading to tenosynovitis. Once a figure skater develops Achilles tenosynovitis, the problem can be difficult to resolve because the tenosynovium remains sensitive to the pressure from the boot (2).
Stress Fractures
Some figure skaters may also suffer from stress fractures due to overuse (such as repeatedly practicing the same jumping skill). Stress fractures can occur to the metatarsals; the long bones of the foot between the phalanges (the toes) and the tarsals. Any metatarsal may experience a stress fracture, but occur most commonly to the first and second metatarsal, the fourth and fifth metatarsals and in the tarsal navicular (3). The mechanism of injury is overuse through repeated loading of the foot (4). According to Bradley, “The metatarsals are frequently loaded when the foot "toes in" on toe jumps (toe loop, flip or lutz jumps). The navicular is usually overloaded on the take-off foot” (3).
Additional risk factors for metatarsal stress fractures include any combination of the following: sudden increases in intensity or duration of activity, decreases in the amount of rest and recovery, changes in training surface, changes in footwear, inadequate nutrition, low bone mass, and length differences between the first and second metatarsals (4,5).
Knee Injuries
In addition to foot and ankle injuries, figure skaters can develop pain and dysfunction at the knee. The most common complaints are patellofemoral syndrome and Osgood-Schlatters disease (2). Acute injury caused by falling on one’s knees also occurs, however overuse injuries are more prevalent. Of note, injuries to the anterior cruciate ligament (ACL) and meniscus are relatively low (2).
Patellofemoral Syndrome
Patellofemoral syndrome is characterized by a dull aching pain in the front of the knee and is defined as “pain in the knee region that is provoked or accentuated by actions that involve motion at the patellofemoral joint and/or increase pressure of the patella against the femoral condyles”(6). One of the most commonly accepted causes of patellofemoral syndrome is abnormal tracking of the patella within the femoral trochlea. In other words, muscles around the hips (abductors) and knees do not function optimally (poor neuromuscular control and muscle imbalance) to maintain proper tracking of the kneecap.
Osgood-Schlatter Disease
According to Mayo Clinic, “Osgood-Schlatter disease can cause a painful lump below the kneecap in children and adolescents experiencing growth spurts during puberty.” Osgood-Schlatter disease is common in children who participate in sports involving jumping and running such as figure skating, basketball, and ballet. Boys are more often affected by Osgood-Schlatter disease than girls; however, that gap is narrowing as more girls are participating in organized sport (7). Symptoms of Osgood-Schlatter disease include swelling, pain, and tenderness of the bony prominence on the tibia just below the kneecap (tibial tubercle).
Corrective Exercise Strategies
If a figure skating athlete presents pain or dysfunction the fitness professional should never attempt to diagnose the problem but rather refer his or her client to a qualified medical professional. However, utilizing various movement screens, fitness professionals should assess their clients to identify potential muscles imbalances (muscle weakness and muscle tightness) and faulty movement patterns and subsequently implement a corrective exercise strategy to proactively address these concerns. For a list of comprehensive movement screens see NASM’s Corrective Exercise Specialist.
Following a comprehensive fitness assessment (including a battery of movement screens), fitness professionals should implement a corrective exercise program that is individualized for their client:
- Step 1: Inhibitory techniques (self-myofascial release) should be used to decrease tension and effects of latent trigger points of the overactive muscles surrounding the affected area and adjacent segments.
- Step 2: Static stretching should be performed for a minimum of 30-60 seconds on identified overactive muscles to help facilitate optimal joint ROM and muscle extensibility.
- Step 3: Isolated strengthening exercises should be used to facilitate identified underactive muscles. Auditory and tactile feedback while performing these exercises can also help develop neuromuscular activation and help the client “feel” the proper movement pattern and activation of the muscle.
- Step 4: Lastly, exercises are progressed by incorporating activities that integrate the entire kinetic chain (multijoint, compound movements) to enhance neuromuscular efficiency and coordination.
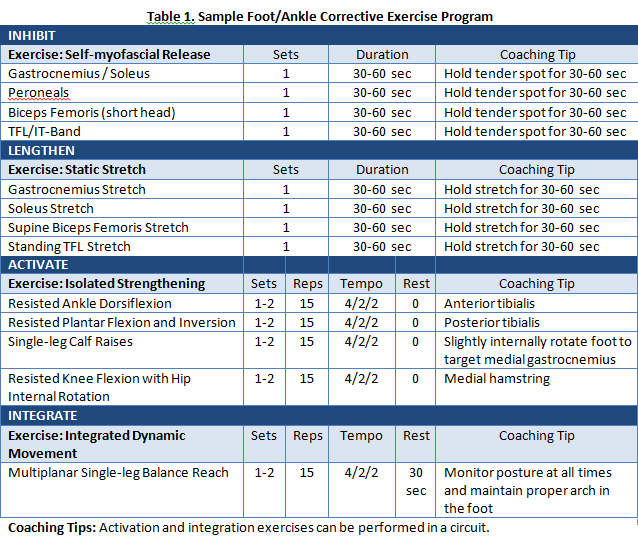
Table 1 is an example of a corrective exercise program for an athlete with foot/ankle dysfunction. In most cases restoring adequate ankle dorsiflexion is paramount (4). Stretching should be relatively pain-free and can be performed several times a day. Other exercises should be incorporated to strengthen the musculotendinous structures of the foot and improve proprioception. Calf strengthening can be done through heel raises and can be paired with exercises to strengthen the anterior tibialis, posterior tibialis and medial hamstrings. For more examples of corrective exercise programs (such as for knee or shoulder impairments), refer to NASM’s Corrective Exercise Specialist.
References
- Fortin JD, Roberts D. Competitive figure skating injuries. Pain Physician. 2003 Jul;6(3):313-8.
- Jaworski CA, Ballantine-Talmadge S. On thin ice: preparing and caring for the ice skater during competition. Curr Sports Med Rep. 2008 May-Jun;7(3):133-7.
- Bradley MA. Prevention and treatment of foot and ankle injuries in figure skaters. Curr Sports Med Rep. 2006 Sep;5(5):258-61.
- Krivickas LS. Anatomical factors associated with overuse sports injuries. Sports Med. 1997; 24:132-46.
- Chuckpaiwong B, Cook C, Pietrobon R, Nunley JA. Second metatarsal stress fracture in sport: comparative risk factors between proximal and non-proximal locations. Br J Sports Med. 2007; 41:510-4.
- Arnoldi C. The patellar pain syndrome. Acta Orthopedica Scandinavica. 1991; 244:62.
- Mayo Clinic Staff. Osgood-Schlatter disease. http://www.mayoclinic.org/diseases-conditions/osgood-schlatter-disease/basics/definition/con-20021911. Accessed January 29, 2018.